by Irish Referral Agency | Oct 10, 2025 | News
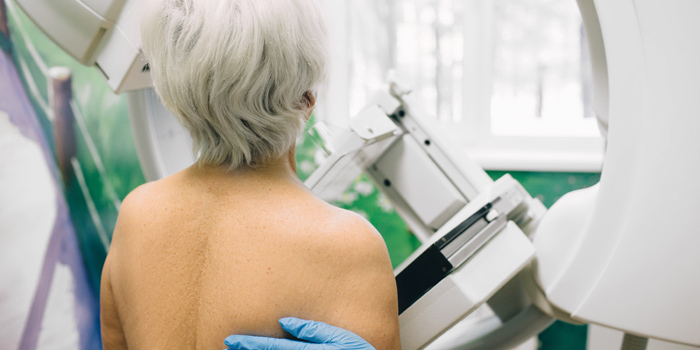
It’s a question many adult children ask as their mothers age: Is Mom too old to need a mammogram? After decades of routine screenings, it’s natural to wonder whether the benefits still outweigh the risks. But the answer isn’t one-size-fits-all, and it’s more nuanced...
by Irish Referral Agency | Sep 30, 2025 | News
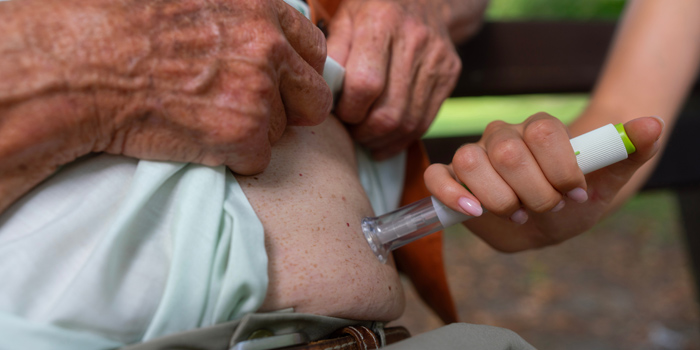
With nearly 1 in 3 adults over 65 living with diabetes, caregivers play a vital role in ensuring insulin is stored, handled, and administered safely. Whether you’re supporting a parent, spouse, or client, understanding the basics of insulin management can help prevent...

by Irish Referral Agency | Sep 20, 2025 | News
Maintaining personal hygiene is more than a daily task. It is a cornerstone of dignity, health, and emotional well-being for seniors. As aging introduces new challenges, caregivers and loved ones must adjust their routines to ensure comfort, safety, and dignity. From...

by Irish Referral Agency | Sep 10, 2025 | News
Building Brain Resilience Through Everyday Activities As we age, many of us become more aware of changes in memory, attention, and mental sharpness. But aging doesn’t have to mean cognitive decline. In fact, research into “cognitive reserve” offers a hopeful message:...

by Irish Referral Agency | Aug 30, 2025 | News
Recent research continues to strengthen the connection between hearing loss and dementia, suggesting that hearing health may play a pivotal role in cognitive aging. While hearing aids are not a cure for dementia, emerging evidence indicates they may help slow its...

by Irish Referral Agency | Aug 20, 2025 | News
As we age, our health and well-being become top priorities. Many senior citizens rely on health care, home care, and other essential services to maintain their quality of life. One often overlooked but important aspect of accessing these services is ensuring that...

by Irish Referral Agency | Aug 10, 2025 | News
November is National Home Care and Hospice Month, a time to honor the dedicated professionals who provide compassionate care to those in need. Home care and hospice workers play a crucial role in the healthcare system, offering support and comfort to patients and...

by Irish Referral Agency | Jul 30, 2025 | News
The desire to age in place – to remain in the familiar surroundings of one’s own home – becomes a heartfelt aspiration for many as our parents enter their golden years. This decision brings a sense of independence and comfort. However, it requires a thoughtful...

by Irish Referral Agency | Jul 20, 2025 | News
When we think about hearing loss in older adults, it’s easy to focus on the obvious: the need to turn up the TV, missed phone calls, or the occasional “What did you say?” But the impact of untreated hearing loss goes far deeper, affecting emotional health, cognitive...

by Irish Referral Agency | Jul 10, 2025 | News
Just as people put the task of checking their smoke alarm batteries on some sort of regular calendar, reviewing your will is something that should be done regularly, as well. Life circumstances and legal changes make doing so critically important. So, as the new...











